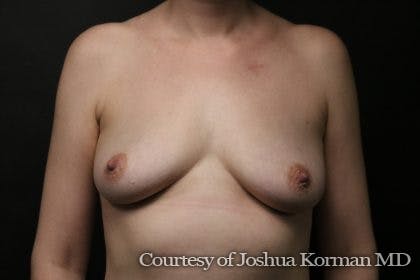
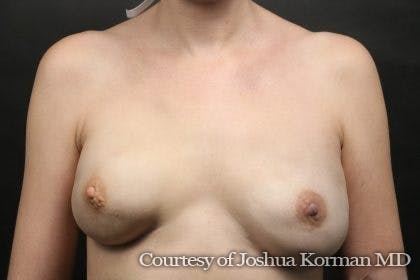
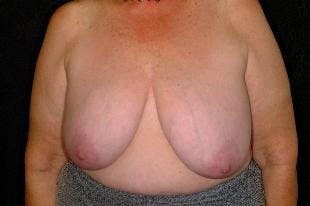
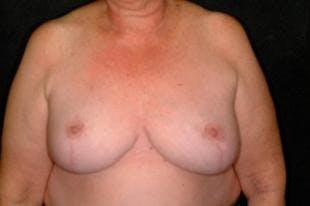
Breast reconstruction is a procedure that rebuilds a patient’s breasts, most often after a mastectomy. Patients can choose a breast reconstruction immediately following a mastectomy or after time spent recovering.
What Is Breast Reconstruction?
Some patients might be self-conscious about their appearance after a mastectomy. Other patients may worry about having two surgical procedures done in quick succession. Patients should feel empowered to choose when to undertake breast reconstruction. Breasts can be rebuilt immediately following a mastectomy or even as part of a single procedure. Reconstruction of the breast can also be done at a later date if the patient decides on that course of action.
Different circumstances and concerns may require different solutions. There are two primary types of procedures used to reconstruct a patient’s breast after a mastectomy: implant reconstruction and flap reconstruction. Flap reconstruction may also be called autologous reconstruction. The style of breast reconstruction that best suits an individual patient will vary. A consultation with a plastic surgeon will help determine which technique will best help you achieve your aims.
- Breast Reconstruction with Implants – First an expander is placed. Then, an implant of saline or silicone is placed to recreate the shape of the breast.
- Flap Reconstruction – Flap or autologous reconstruction is when tissue from other parts of the body is used to restore the breast.